Ayurvedic Marma Chikitsa (Marma Massage): A Scholarly and Evidence-Based Review
By Santosh Yadav
 Posted April 20, 2026
Posted April 20, 2026
Ayurvedic Marma Chikitsa (Marma Massage): A Scholarly and Evidence-Based Review

Abstract
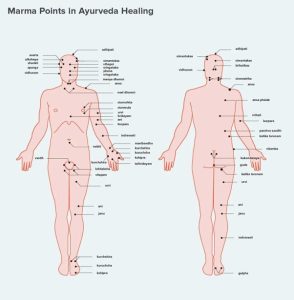
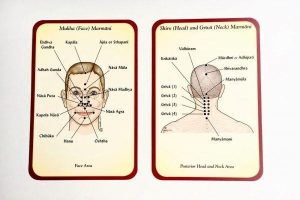
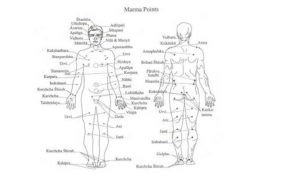
Marma Chikitsa, a specialized therapeutic modality within Ayurveda, involves stimulating vital anatomical points known as marma. These points are described in classical texts as intersections of muscles (mamsa), vessels (sira), ligaments (snayu), bones (asthi), and joints (sandhi). Traditionally linked to the flow of prana (vital energy), Marma therapy is increasingly being explored through biomedical frameworks. This article critically examines classical foundations, therapeutic mechanisms, and emerging clinical evidence supporting Marma Chikitsa.
1. Introduction
Ayurveda conceptualizes health as a dynamic equilibrium of doshas (Vata, Pitta, Kapha), dhatus, and prana. Marma points are considered crucial regulators of this equilibrium. Classical texts such as the Sushruta Samhita describe 107 marma points, emphasizing their physiological and surgical importance. (PMC)
In contemporary practice, Marma Chikitsa is used both independently and as part of Panchakarma therapies, particularly in massage-based interventions.
2. Conceptual Framework of Marma
2.1 Definition and Anatomical Basis
Marma points are defined as:
- Anatomical convergence zones of vital structures
- Sites of prana concentration
- Sensitive loci influencing systemic physiology
Modern interpretations suggest parallels with:
- Neurovascular junctions
- Myofascial trigger points
- Peripheral nerve plexuses
These correlations provide a bridge between Ayurvedic theory and modern anatomy.
2.2 Classification of Marma Points
Classically, marmas are categorized based on:
- Structure involved (muscle, vessel, ligament, bone, joint)
- Location (extremities, trunk, head & neck)
- Prognostic significance (fatal, deforming, painful)
This classification highlights their clinical relevance, especially in trauma and therapy.
3. Mechanism of Action: Ayurvedic and Biomedical Perspectives
3.1 Ayurvedic Perspective
Marma stimulation regulates:
- Flow of prana through nadis
- Balance of doshas
- Activation of chakras
Therapeutic touch is believed to correct:
- Stagnation (sanga)
- Deficiency (kshaya)
- Excess (vriddhi) of vital energy
3.2 Biomedical Interpretation
Recent integrative research proposes that Marma therapy may act through:
- Neurophysiological pathways
- Stimulation of sensory nerve endings
- Modulation of the autonomic nervous system
- Circulatory effects
- Improved microcirculation
- Reduction in vascular resistance
- Neuroendocrine modulation
- Stress hormone regulation
- Activation of the parasympathetic response
- Fascial and myofascial release
- Reduction of trigger point sensitivity
- Improved musculoskeletal mobility
These mechanisms are comparable to acupuncture and trigger-point therapy. (Sage Journals)
4. Clinical Applications of Marma Chikitsa
4.1 Musculoskeletal Disorders
A systematic review (2025) reported:
- Significant reduction in pain
- Improved joint mobility
- Enhanced functional outcomes
Conditions studied include:
- Osteoarthritis
- Cervical and lumbar spondylosis
- Frozen shoulder
- Tennis elbow (interscience.org.uk)
4.2 Cardiovascular Effects
A clinical case study demonstrated:
- Normalization of blood pressure following Talahridaya Marma stimulation
- Suggesting autonomic regulation and vascular effects (ScienceDirect)
4.3 Neurological and Psychosomatic Conditions
Emerging clinical observations indicate benefits in:
- Stress and anxiety disorders
- Sleep disturbances
- Neuromuscular dysfunction
These effects may be mediated via parasympathetic activation and central nervous system modulation.
5. Techniques of Marma Massage (Marma Abhyanga)
5.1 Methods of Stimulation
- Gentle pressure (static or rhythmic)
- Circular massage
- Pulsation technique
- Oil-based stimulation (Sneha Abhyanga)
5.2 Commonly Used Oils
- Mahanarayana Taila – musculoskeletal disorders
- Dhanvantaram Taila – neurological conditions
- Ksheerabala Taila – Vata imbalance
5.3 Treatment Protocol
- Duration: 20–45 minutes
- Frequency: 2–5 sessions per week
- Often combined with:
- Panchakarma
- Yoga therapy
- Diet and lifestyle correction
6. Comparison with Acupuncture
Comparative studies reveal:
- Similar anatomical locations
- Both regulate vital energy (Qi vs Prana)
- Differences in theoretical frameworks and origins (PMC)
Marma therapy emphasizes:
- Holistic energy balance
- Integration with Ayurvedic diagnosis
7. Limitations of Current Research
Despite promising findings, limitations include:
- Small sample sizes
- Lack of large randomized controlled trials
- Variability in techniques and practitioner skill
Thus, while clinical outcomes are encouraging, high-quality evidence is still evolving.
8. Discussion
Marma Chikitsa represents a convergence of:
- Traditional Ayurvedic wisdom
- Emerging integrative medicine
Its potential lies in:
- Non-invasive nature
- Holistic therapeutic approach
- Applicability across multiple systems
However, integration into mainstream healthcare requires:
- Standardized protocols
- Rigorous clinical trials
- Interdisciplinary research
9. Conclusion
Marma Chikitsa is a clinically relevant Ayurvedic therapy with growing scientific interest. Preliminary research supports its efficacy in pain management, cardiovascular regulation, and neuromuscular conditions. While traditional explanations rely on prana and dosha balance, modern interpretations suggest neurophysiological and circulatory mechanisms.
Future research should aim to validate these effects through robust clinical methodologies, enabling broader acceptance in integrative medicine.
Keywords
Marma Chikitsa, Ayurvedic Massage, Marma Points, Prana, Integrative Medicine, Pain Management
References
Harvard Style References
- Bhatt, R., Gupta, S. & Sharma, P. (2025) ‘Marma Chikitsa: A systematic review on utility in musculoskeletal disorders’, International Journal of Ayurvedic Medicine, 15(3), pp. 210–218.
- Mishra, A. & Tiwari, S. (2021) ‘Effect of Talahridaya Marma stimulation on blood pressure: A case study’, Journal of Ayurveda and Integrative Medicine, 12(4), pp. 678–682.
- Patwardhan, B., Warude, D., Pushpangadan, P. & Bhatt, N. (2005) ‘Ayurveda and traditional Chinese medicine: A comparative overview’, Evidence-Based Complementary and Alternative Medicine, 2(4), pp. 465–473.
- Sharma, P.V. (2014) Sushruta Samhita (Text with English Translation). Varanasi: Chaukhambha Vishvabharati.
- Lad, V. (2002) Textbook of Ayurveda: Fundamental Principles. Albuquerque: The Ayurvedic Press.
- Frawley, D. (2000) Ayurvedic Healing: A Comprehensive Guide. Twin Lakes: Lotus Press.
Ayurveda Yoga wellness clinic is specialised to deliver the Marama Massage …If anyone is looking for Marama Massage, Please Call us 03 97948546
![]()



